Plantar fasciitis: what is it?

Heel pain is frequently brought on by plantar fasciitis.
The plantar fascia, a strong, thick band of tissue, maintains the foot arch. The foot may feel sore and have trouble moving if this tissue is injured or inflamed.
About 80% of occurrences of heel discomfort are caused by plantar fasciitis, according to the National Institute for Health and Care Excellence. According to estimates, 10% of people will have this issue at some point in their lives.
We give a general review of plantar fasciitis in this article, covering its causes, risk factors, symptoms, and treatments. We also go into when someone should visit a doctor.
Why does plantar fasciitis occur?

The plantar fascia's job is to cushion the foot from the force of standing, walking, and running. The plantar fascia can be harmed by excessive pressure because this area of the body is frequently used.
There isn't always just one reason why someone gets plantar fasciitis. There are a number of risk factors that can raise a person's risk of getting the illness. These consist of:
- having flat feet, high arches, or tight calf muscles
- being overweight or obese, being pregnant, or any of a number of other conditions that increase strain on the foot.
- age, since plantar fasciitis is more common in adults between the ages of 40 and 60 years.
- having specific health issues, such arthritis
- constantly standing for long periods of time
- frequently wearing high heels
In comparison to men, women are more prone to have plantar fasciitis. It is unclear why it’s more common in women than in males although it could be because of several risk factors for the illness, like being pregnant and wearing shoes that are not supportive.
The problem typically arises as a result of repeated pressure or impact, which can harm the tissue in the foot over time.
Symptoms
From the tips of the toes to the back of the heel, the plantar fascia runs down the sole. Small tears in the tissue may result from excessive pressure on this area of the foot. Pain, stiffness, and inflammation are brought on by this injury.
Pain in the plantar fascia is the most typical sign of plantar fasciitis. The area of the heel where the pain is most prevalent can seem as though the tissue is tearing.
Over time, the pain could come on gradually. After a time of relaxation, such as first thing in the morning or following a lengthy trip, it could be worse. Alternatively, the discomfort could get worse following exercise or activities.
On the base of the heel bone are tiny, bony growths known as heel spurs. Heel spurs do not cause the pain associated with plantar fasciitis, contrary to popular belief.
A home remedy
Exercises and stretches that target the muscles in the foot or leg can help reduce plantar fasciitis discomfort and promote recovery. Exercises like folding a towel between the toes and picking up marbles with the toes are included in this list, along with foot flexes and calf stretches.
Resting the foot, applying cold compress to the affected area, bandaging it, and elevating it on cushions or a low stool can all be beneficial. Anti-inflammatory medications that are non-steroidal can lessen pain and swelling. Some individuals may discover that foot massage also reduces foot pain.
It may take a while to recover. One may be able to walk properly and pain-free after a week or two of rest and home treatment. The majority of patients with plantar fasciitis heal fully within a year.
Alterations in your lifestyle

Simple lifestyle adjustments can aid in the foot's recovery and stop the recurrence of plantar fasciitis.
The daily strain of standing and walking on the feet can be lessened by using supportive footwear that is comfortable. An overview of selecting the appropriate footwear is provided by the American Academy of Orthopaedic Surgeons.
Athletic shoes should be replaced when they become worn. A shoe's sole becomes less supportive and less able to cushion the shock when the foot strikes the ground as it gets thinner.
To help to prevent injury, it is important to select low-impact forms of exercise. Running on the sidewalk puts more stress on the foot and knee joints than jogging on a soft surface like grass. Both yoga and swimming can increase flexibility and strength with little to no negative effects on the body.
Reduced pressure on the feet can also be achieved by maintaining a healthy weight. Healthy eating and regular, mild exercise are good weight-management strategies.
Treatments
Rest and self-care at home are frequently the most successful treatments for plantar fasciitis. In the event that natural cures are unsuccessful, a doctor might suggest extra therapy. The majority of therapies are nonsurgical, and doctors only advise surgery if nonsurgical measures have failed after a year.
Orthotics
A support or device known as an orthotic can assist with musculoskeletal issues, which are issues involving the bones, muscles, and ligaments. Plantar fasciitis discomfort can be relieved by wearing supportive footwear and employing orthotics, such as cushioned inserts and heel supports. These lessen the force that the foot experiences when standing or walking.
A night splint
Normal sleeping positions involve relaxed, downward-facing feet. The plantar fascia becomes more taut in this posture as the heel relaxes. Additionally, it may make the calf muscles tighter, which can make the discomfort in the arch worse. A night splint can be used by people to keep their foot flexed at night.
Physical therapy
Stretching the muscles through physical therapy can increase range of motion, lessen pain, and promote recovery. Inflammation and pain can both be reduced with massage treatment.
Anti-inflammatories
An anti-inflammatory drug is called cortisone. Injections of cortisone into the tissue might lessen discomfort and inflammation. To lessen the danger of side effects, it is preferable to restrict the number of injections.
Shockwave treatment
A non-surgical procedure that might help the process of healing is extracorporeal shockwave therapy. Although it is non-invasive and low risk treatment, additional research is required to determine its efficacy.
Surgery
A doctor might advise surgery if none of these therapies work. Although there is a mild chance of consequences from plantar fasciitis surgery, these can include discomfort or nerve damage. There are two primary surgical options:
- The plantar fascia is less stressed as a result of the gastrocnemius recession, which lengthens the calf muscles to expand the range of motion in the ankle. The surgeon will either do an open procedure or a minimally invasive procedure, which could shorten the recuperation period.
- In order to release tension, a surgeon must make a cut in the plantar fascia. The technique is more suited for people whose ankles have a good range of motion.
When to seek medical attention
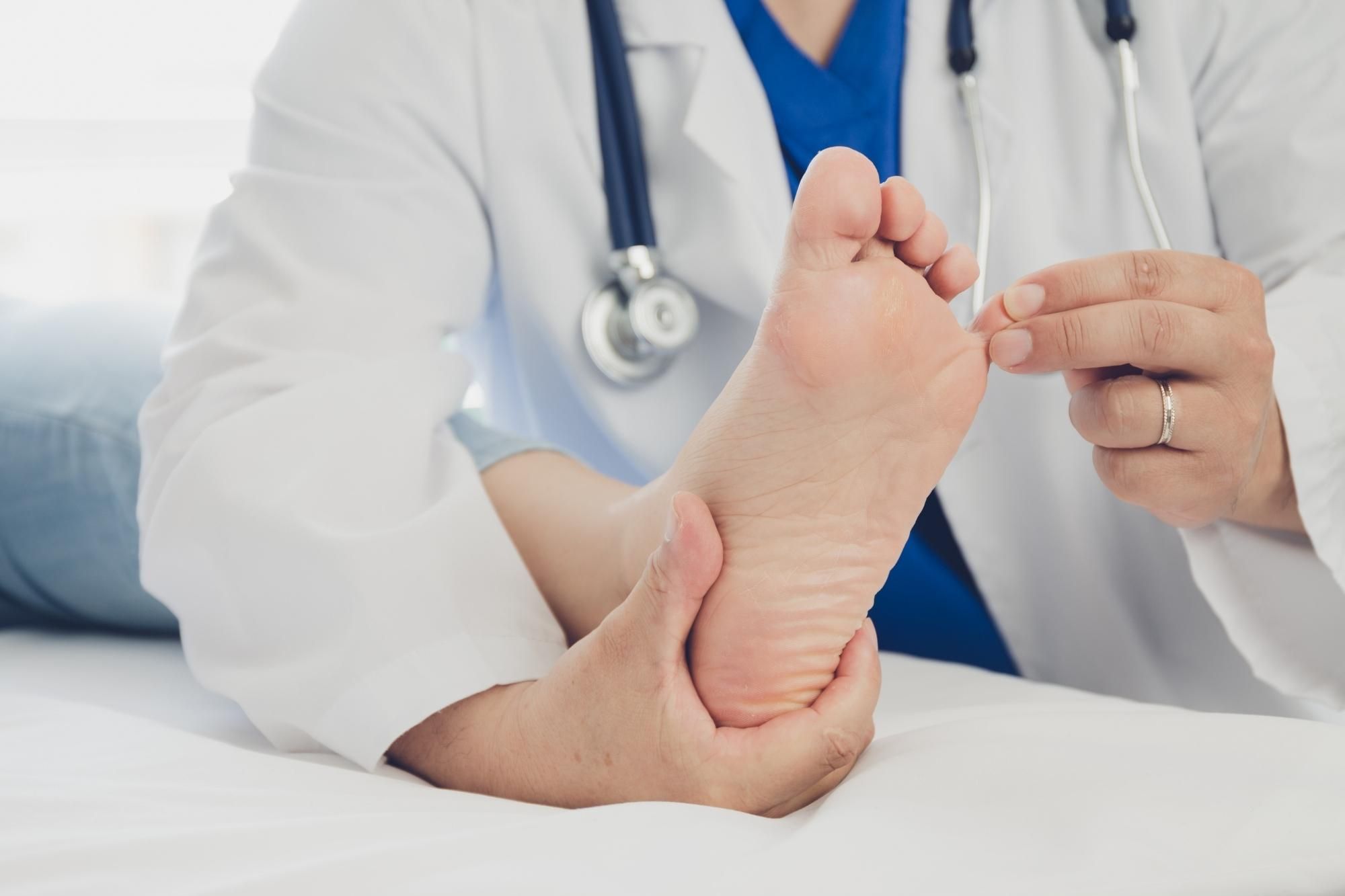
It is crucial to see a doctor if pain persists after attempts at self-care. Ignoring plantar fasciitis can result in continuous pain and even damage to the foot's structural components.
A patient will typically be questioned by the doctor about their symptoms, medical history, and any possible lifestyle choices that may have contributed to the issue. They might also want to know the precise spot where the pain is, whether it gets worse after exercise or at particular times of the day.
The doctor will then perform a foot examination to check for plantar fasciitis symptoms. These may consist of:
- front of the heel bone discomfort or soreness
- pain that gets worse as the plantar fascia is pressed upon or flexed
- ankle movement with a restricted range
The doctor will be able to suggest treatments after making a diagnosis.
Conclusion
Plantar fasciitis can result in severe pain and make it difficult to move the foot normally. However, the majority of patients fully recover from the illness.
Home remedies and easy lifestyle modifications are typically beneficial in treating plantar fasciitis. By exercising with little impact, dressing appropriately, and maintaining a healthy weight, one can lessen the risk factors.
Sources: